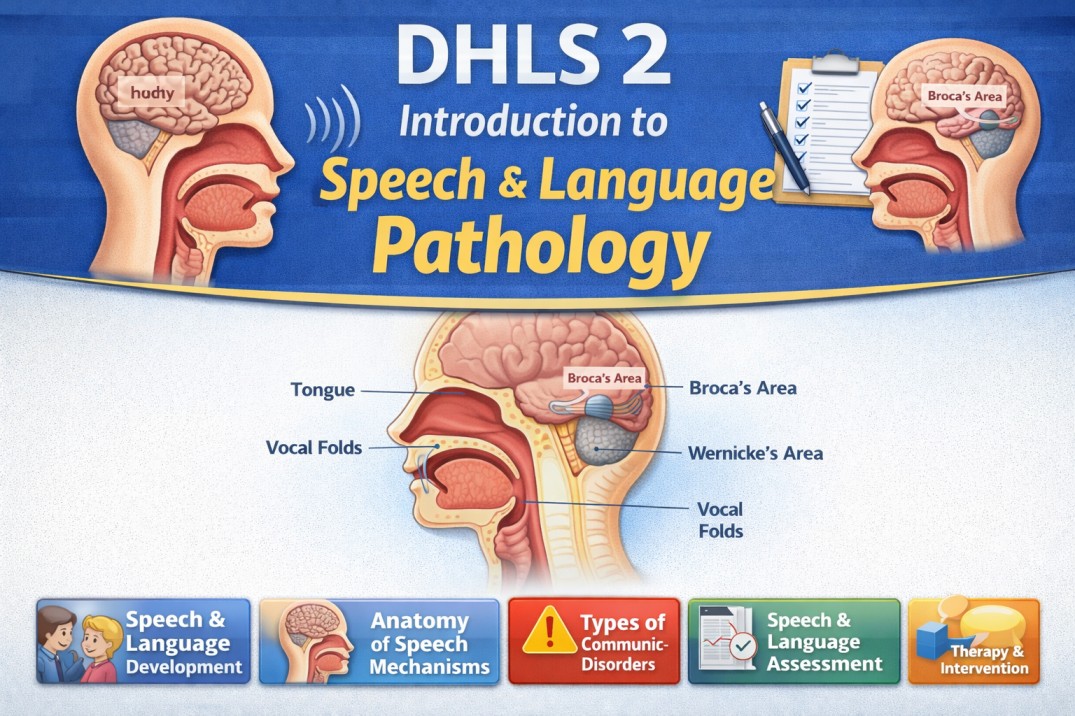
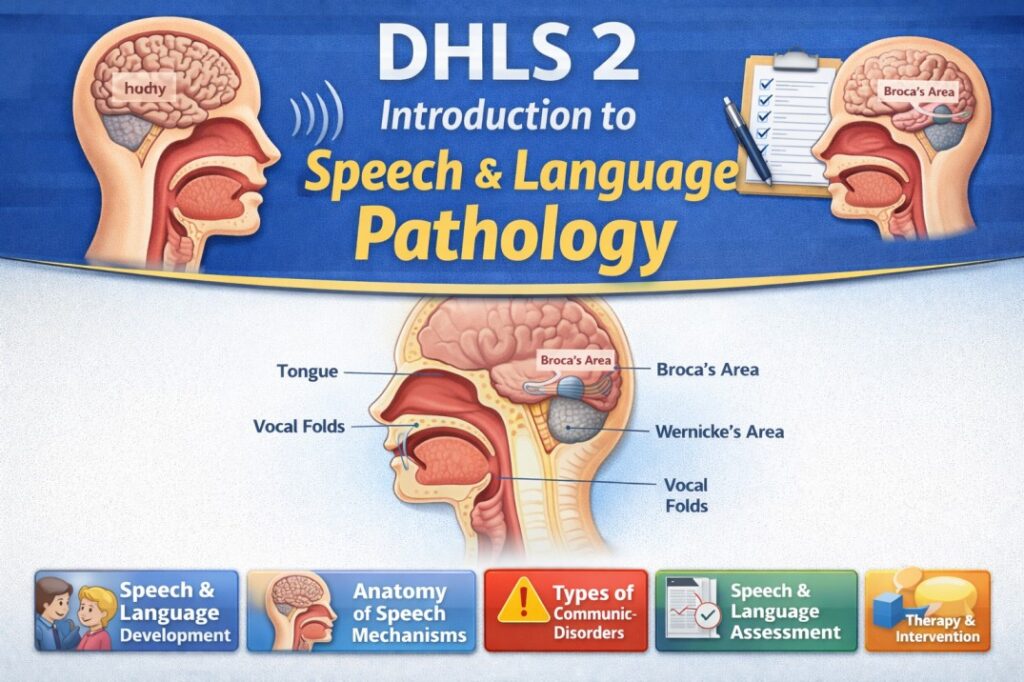
Speech is a complex motor activity that requires the coordinated and synchronized functioning of multiple systems. The process begins with the respiratory system, which provides the airflow needed for speech production. The expiratory air from the lungs acts as the basic source of sound.
This airflow is then modified by the phonatory system at the level of the larynx, where the vocal cords vibrate to produce voice (phonation). The produced voice is further shaped by the resonatory system, which includes the larynx, pharynx, oral cavity, and nasal cavity. These structures help in giving quality and richness to the sound.
Finally, the articulatory system, consisting of organs such as the lips, tongue, palate, and velopharyngeal mechanism, modifies the sound into distinct speech sounds. These sounds are organized in a proper sequence according to the rules of language.
All these systems—respiratory, phonatory, resonatory, and articulatory—are controlled and coordinated by the nervous system (both central and peripheral) to ensure accurate speech production and understanding during daily communication.
Table of Contents
ToggleSystem involved in speaking
There are several systems in our body help in speech production. These include:
- Nervous system
- Respiratory system
- Phonatory system
- Articulatory
- Resonatory system
Speech is a unique ability of human beings, mainly because of the human brain and nervous system, which control and coordinate all activities required for speaking. Unlike animals, humans can understand, process, and produce meaningful speech due to this advanced system.
The respiratory system plays an important role by providing the airflow needed for speech. When we produce sounds like “ssss,” we can feel the air coming out, which shows that speech depends on expiratory air from the lungs.
The phonatory system is responsible for producing voice. When we say sounds like “aaaa,” we can feel vibrations in our neck. These vibrations are produced by the vocal folds in the larynx, which are essential for voiced speech. Whispering, which lacks vocal fold vibration, shows that without proper phonation, speech becomes weak and tiring.
The articulatory system includes organs like the tongue, lips, teeth, and palate, which help in shaping sounds into clear speech. For example, elderly people without teeth or young children with developing speech organs may have unclear pronunciation, showing the importance of articulators.
Thus, speech depends on the proper functioning of the nervous system, respiratory system, phonatory system, and articulatory system, all working together to produce clear and meaningful communication.
Structure and functions of speech mechanism
Nervous system
When we have a desire to speak, the nervous system becomes active and controls the entire speech process. It consists of the brain and nerves, with the brain located inside the skull. The brain has two hemispheres—left and right, each divided into four lobes: frontal, temporal, parietal, and occipital lobes. Specific areas in these lobes are responsible for speech.
The Wernicke’s area in the temporal lobe helps in understanding language, selecting words, and organizing them in proper order. This information is then sent to the Broca’s area and motor areas in the frontal lobe, which convert the message into motor commands for speech production. These commands are transmitted through nerves to different speech-related muscles. Thus, the nervous system acts like a commander, controlling all other systems involved in speech.
The brain communicates with the body through 12 pairs of cranial nerves, which carry sensory and motor information.
- Motor nerves send signals from the brain to muscles and glands.
- Sensory nerves carry information from sensory organs (like tongue, skin, etc.) to the brain.
The basic unit of the nervous system is the neuron, which transmits nerve signals. A neuron consists of:
- Cell body (soma) → contains nucleus
- Dendrites → receive signals
- Axon → carries signals away from the cell body
- Synapse → gap where signals pass to the next cell
The axon is covered by myelin, which helps in faster transmission of signals. Nerve signals can travel very fast (up to 200 mph), allowing quick coordination of speech.
In summary, the nervous system plays a central role in speech production by planning, controlling, and coordinating all activities through the brain, nerves, and neurons.
Respiratory system
The respiratory system consists of structures involved in breathing (inspiration and expiration). Air enters through the nostrils, passes through the nasopharynx and oropharynx, then through the glottis into the trachea, and further into the bronchi and bronchioles, finally reaching the alveoli. The alveoli are tiny air sacs (about 300 million) where gas exchange takes place. Oxygen enters the blood, and carbon dioxide is removed.
Breathing involves the diaphragm and intercostal muscles. During inspiration, the diaphragm contracts and moves downward while the ribs move upward and outward, increasing the chest cavity volume and allowing air to enter the lungs. During expiration, these actions reverse, and air is pushed out due to the natural elasticity of the lungs. At rest, humans breathe about 15–18 times per minute, exchanging around 500 ml of air, while maximum breathing capacity (vital capacity) can reach about 4 liters.
| Component | Atmospheric Air (%) | Expired Air (%) |
| N2 (plus inert gas) | 72.62 | 74.9 |
| O2 | 20.85 | 15.3 |
| CO2 | 0.03 | 3.6 |
| H2O | 0.5 | 6.2 |
| Total | 100.0 | 100.0 |
The composition of air changes during breathing. Oxygen decreases while carbon dioxide and water vapor increase in expired air. The medulla oblongata in the brain controls breathing, mainly responding to increased carbon dioxide levels. Additionally, receptors in the carotid arteries respond to low oxygen levels. Locally, bronchioles adjust airflow by dilating or constricting based on carbon dioxide concentration.
Respiration is essential for speech production, as speech is produced using modified air. Unlike quiet breathing (equal inspiration and expiration), in speech, inspiration is shorter and expiration is longer, allowing controlled airflow. The respiratory system acts like a pump, providing the energy (air pressure of about 5–8 cm of H₂O) required for speech. This airflow is then modified by the laryngeal and resonatory systems to produce different speech sounds.
Thus, the respiratory system provides the basic energy source for speech, making it a crucial component in speech production.
Phonatory system
The laryngeal or phonatory system consists of the larynx (voice box), which plays a key role in voice production. The larynx is located at the upper end of the trachea, between the trachea and the oral tract. It lies opposite the 3rd to 6th cervical vertebrae in the neck. Its position varies depending on age, gender, head position, and swallowing, and it is generally higher in women and children than in men.
The size of the larynx differs between males and females. In adult males, it is relatively larger, while in females it is smaller. There is no major difference in size between boys and girls before puberty, but during puberty, the larynx in males grows significantly, especially in the antero-posterior dimension, leading to noticeable voice changes.
The larynx performs both biological and non-biological functions. Biologically, it helps in protecting the airway and in building pressure within the chest for activities like coughing or heavy physical effort. Non-biologically, it is essential for speech production and singing, as it produces voice through the vibration of the vocal folds.
Anatomy of larynx
The larynx is a complex structure made up of bone, cartilages, muscles, membranes, and joints, all working together for voice production and airway protection. The hyoid bone plays an important role in supporting the larynx.
The hyoid bone is a U-shaped single bone located above the thyroid cartilage. It is unique because it is not directly attached to any other bone. Instead, it is suspended by ligaments from the styloid processes of the temporal bones. The hyoid bone is supported by several muscles, which allow it to move in different directions, aiding in speech and swallowing.
Structurally, the hyoid bone has three parts: a central body and two pairs of horns (greater and lesser horns). These horns help in connecting the hyoid bone to the thyroid cartilage.
The larynx also contains six cartilages—three unpaired and three paired—which form its framework and help in various functions like voice production and protection of the airway.
Laryngeal Cartilage
The larynx has a structural framework made up of cartilages, which provide support and shape. These cartilages are connected by ligaments and membranes, allowing them to stay in position while still permitting movement. The movement of these cartilages is controlled by intrinsic and extrinsic muscles, which help in functions like voice production and breathing.
The inner surface of the larynx is lined with a mucous membrane. This lining is continuous with the mucous membrane of the pharynx above and behind, and with that of the trachea below, forming a continuous passage for air.
| Cartilage | Number | Location |
| Epiglottis | single | Behind the hyoid bone and base of the tongue |
| Thyroid | single | Front of the neck in the midline |
| Cricoid | single | Above the trachea; below thyroid cartilage |
| Arytenoids | paired | Rests on the back surface of cricoid cartilage |
| Corniculates | paired | Rests on the arytenoid cartilages |
| Cuneiform | paired | Embedded in aryepiglottic folds |
The thyroid cartilage
The thyroid cartilage is the largest, shield-shaped cartilage of the larynx and forms the main protective structure of the voice box. It is made up of two flat plates (laminae) that join in the midline in front. At the upper part, these laminae do not completely meet, leaving a thyroid notch which can be easily felt.
The angle at which the laminae meet differs in males and females—about 90° in males and 120° in females. In males, this sharper angle forms a noticeable projection called the laryngeal prominence or Adam’s apple.
The thyroid cartilage has two projections on each side:
- Superior cornu → long and narrow, curves upward, backward, and medially; attached to ligaments.
- Inferior cornu → shorter and thicker, curves downward and connects with the cricoid cartilage.
Additionally, the thyro-epiglottic ligament is attached to the inner surface of the thyroid notch. The front ends of the vocal ligaments join here to form the anterior commissure tendon, which is clinically important, especially in the spread of certain diseases like carcinoma.
The cricoid cartilage
The cricoid cartilage is a very important structure of the larynx as it is the only complete ring of cartilage in the airway. It forms the lower (inferior) part of the larynx, contributing to the anterior, lateral, and most of the posterior walls.
It is often compared to a signet ring in shape:
- The posterior part is broad and deep, called the lamina
- The anterior part is narrow, called the arch
The cricoid cartilage articulates with the thyroid cartilage through its inferior cornu, allowing rotational movements between them. These movements are important for voice production.
At the back, a vertical ridge is present, which connects to the esophagus muscles. On either side of this ridge are shallow depressions that provide attachment for the posterior cricoarytenoid muscles, which play a key role in opening the vocal folds.
The entire cricoid cartilage is lined with a mucous membrane, ensuring a smooth internal surface for airflow.
The arytenoid cartilage
The arytenoid cartilages are a pair of small cartilages located on the upper and lateral borders of the cricoid lamina. Each arytenoid is shaped like a three-sided pyramid and plays a crucial role in voice production.
Each arytenoid cartilage has two important projections:
- Vocal process (anterior projection) → attached to the vocal folds
- Muscular process (lateral projection) → provides attachment for muscles like posterior and lateral cricoarytenoid muscles
The surface between these projections is divided into two parts:
- Upper fossa → attachment for the vestibular ligament
- Lower fossa → attachment for vocalis and lateral cricoarytenoid muscles
The apex of the arytenoid is directed backward and medially and connects with the corniculate cartilage, which supports the aryepiglottic folds. The medial surfaces are covered with mucous membrane and form part of the boundary of the rima glottidis (opening between vocal folds). The posterior surface is covered by the transverse arytenoid muscle.
The arytenoid cartilages are capable of rotation and side-to-side (medial and lateral) movements, which are essential for opening and closing the vocal folds during breathing and speech. When open, the glottis appears like an inverted “V” shape.
A strong posterior cricoarytenoid ligament helps prevent excessive forward movement of these cartilages.
The corniculate and cuneiform cartilages
The corniculate cartilages are a pair of small, cone-shaped cartilages made of elastic fibrocartilage. They are located at the apex of the arytenoid cartilages and may either articulate with them through a synovial joint or sometimes become fused with them. These cartilages are found within the posterior part of the aryepiglottic folds and help in supporting these folds.
The cuneiform cartilages are also small structures made of elastic fibrocartilage, but they are elongated and rod-like in shape. Each cuneiform cartilage is situated within the margin of the aryepiglottic fold. Their main function is to provide support and maintain the shape of the fold, helping to keep the airway open.
The cartilage of the epiglottis
The epiglottis is a thin, leaf-shaped structure made of elastic fibrocartilage, located above the larynx near the tongue and hyoid bone. It is attached below to the thyroid cartilage by the thyro-epiglottic ligament. Its upper broad part is directed upward and backward, and the top margin is free.
The sides of the epiglottis are connected to the arytenoid cartilages by the aryepiglottic folds, which together with the epiglottis form the anterior boundary of the laryngeal inlet (opening of the larynx). The posterior surface of the epiglottis is smooth and concave, with a small projection called the tubercle. The anterior surface is covered with mucous membrane.
The epiglottis is also connected to the hyoid bone by the hyoepiglottic ligament, and the space around it contains fatty tissue. Its surface has small pits where mucous glands are present.
Functionally, the epiglottis helps in protecting the airway during swallowing by covering the laryngeal opening. However, in humans, it is not absolutely essential, as breathing, swallowing, and speaking can still occur even if it is damaged.
Joints/ligaments of larynx
The cartilages of the larynx are connected to each other by joints, muscles, and membranes, forming a stable yet flexible structure for speech and breathing. These connections help in movement, support, and coordination of the laryngeal framework.
Extrinsic Ligaments: Extrinsic ligaments connect the larynx to surrounding structures like the hyoid bone and trachea:
- The thyrohyoid membrane connects the thyroid cartilage to the hyoid bone. It is made of fibroelastic tissue and is strengthened by the median thyrohyoid ligament (in the center) and lateral thyrohyoid ligaments (on the sides).
- The cricotracheal ligament connects the cricoid cartilage to the first tracheal ring.
- The hyoepiglottic ligament connects the epiglottis to the hyoid bone.
Intrinsic Ligaments: Intrinsic ligaments connect the laryngeal cartilages to each other and strengthen the joints. They form a fibroelastic membrane beneath the mucous lining, providing an internal framework.
This membrane is divided into two parts:
- Upper Part (Quadrilateral Membrane): 1. Extends between the epiglottis and arytenoid cartilages. 2. Upper margin forms the aryepiglottic fold (boundary of laryngeal inlet). 3. Lower margin forms the vestibular ligament, which supports the false vocal cords.
- Lower Part (Conus Elasticus / Cricovocal Membrane): 1. Thicker and rich in elastic fibers. 2. Extends from the cricoid cartilage to the thyroid and arytenoid cartilages. 3. Its upper free edge forms the vocal ligament, which is the framework of the true vocal cords. 4. The cricothyroid ligament (anterior thickening) connects the cricoid and thyroid cartilages.
| Joints/ligaments | Connects | Action |
| Crico-thyroid ligament and joints | Thyroid to Cricoid | Helps in changing the pitch of voice |
| Crico-arytenoid joints and fragments | Cricoid to Arytenoid | Important for opening and closing of vocal folds |
| Vestibular ligaments | Arytenoids to Thyroid | Helps in changing the pitch of voice |
| Vocal ligaments | Arytenoids to Thyroid | Helps in changing the pitch of voice |
The interior of the larynx
The laryngeal cavity extends from the pharynx at the laryngeal inlet to the lower border of the cricoid cartilage, where it continues into the trachea. It is divided into three main parts by the vestibular and vocal folds: the superior vestibule, the middle part (ventricle/sinus), and the subglottic space.
The laryngeal inlet forms the upper opening of the larynx and is bounded anteriorly by the epiglottis, laterally by the aryepiglottic folds, and posteriorly by the arytenoid cartilages. The superior vestibule lies between the inlet and the vestibular folds and narrows as it goes downward. Its walls are formed by the epiglottis, arytenoids, and aryepiglottic folds.
The middle part of the cavity lies between the vestibular folds (false vocal cords) and vocal folds (true vocal cords). On each side, it opens into a recess called the laryngeal ventricle, from which a pouch called the saccule extends upward. The saccule contains mucous glands that help in lubricating the vocal folds for smooth voice production.
The subglottic space extends from the vocal folds to the lower border of the cricoid cartilage and continues into the trachea. The space between the vestibular folds is called the rima vestibuli, while the space between the vocal folds is called the rima glottidis (glottis), which is essential for voice production and airflow.
The vestibular folds are thick and protective, while the vocal folds are thin, white, and responsible for producing sound. They are made of mucous membrane, ligaments, and muscles and can stretch and vibrate to produce voice.
Additionally, spaces like the pre-epiglottic and paraglottic spaces are present in the larynx and are clinically important, especially in the spread of tumors.
- Epithelium
- Superficial layer of Lamina propria (Reinke’s space)
- Intermediate layer of Lamina propria
- Deep layer of Lamina propria
- Vocalis muscle
The glottis is an elongated opening located between the vocal folds in the front and the vocal processes and bases of the arytenoid cartilages at the back. Its size differs between individuals, with an average length of about 23 mm in males and 16–17 mm in females. In a resting position, the vocal processes are usually about 8 mm apart. The shape of the glottis is not fixed; it changes during breathing and phonation (speech production), allowing control over airflow and sound.
The subglottic space, which is the lower part of the laryngeal cavity, extends from the vocal folds down to the lower border of the cricoid cartilage. The upper part of this space is elliptical in shape, while the lower part becomes wider and circular, continuing into the trachea. It is lined with a mucous membrane, and its walls are formed by the cricothyroid ligament above and the inner surface of the cricoid cartilage below.
The muscles
The muscles of the larynx are divided into two main types based on their function and attachments: extrinsic muscles and intrinsic muscles.
The extrinsic muscles connect the larynx to surrounding structures such as the hyoid bone, skull, and chest. Their main function is to move the entire larynx up or down, which is important during activities like swallowing and speaking.
The intrinsic muscles, on the other hand, are located within the larynx and are responsible for moving the laryngeal cartilages. These movements help in opening, closing, tightening, and relaxing the vocal folds, which are essential for voice production and control of airflow.
Extrinsic muscles
The extrinsic muscles of the larynx are those that connect the larynx to nearby structures and help in moving the larynx as a whole.
The main extrinsic muscles include:
- Sternothyroid muscle → helps in lowering the larynx
- Thyrohyoid muscle → helps in raising or stabilizing the larynx
- Inferior constrictor muscle of the pharynx → assists in swallowing and movement of the larynx
In addition, some muscle fibers from the stylopharyngeus and palatopharyngeus extend forward and attach to the posterior border of the thyroid cartilage, contributing to laryngeal movement.
| Muscle | Origin | Insertion | Action |
| Posterior crico-arytenoid (PCA) | Back surface of Cricoid lamina | Back surface of the muscular process of Arytenoids | Opens the glottis by opening the vocal folds |
| Lateral crico-arytenoid (LCA) | Upper border of the Cricoid arch | Front surface of the muscular process of the Arytenoids | Closes the glottis by closing the vocal folds |
| Cricothyroid (CT) | Front and sides of the Cricoid arch | Thyroid lamina and lower horns of thyroid | Increases the length and tension of the vocal folds |
| Vocalis | Inner surface of the Thyroid | Front surface and vocal process of Arytenoid | Increases tension of vocal folds |
| Transverse arytenoid | Muscular process of one Arytenoid | Muscular process of the opposite Arytenoid | Closing the vocal folds |
| Oblique arytenoid | Muscular process of one Arytenoid | Muscular process of the opposite Arytenoid | Closing the vocal folds |
| Thyroarytenoid | Inner surface of the Thyroid | Front surface and vocal process of Arytenoid | Relaxes the vocal folds |
The larynx is connected to the hyoid bone by the thyrohyoid membrane, so any muscle that moves the hyoid bone will also affect the position of the larynx.
Muscles that elevate (raise) the hyoid bone—such as the mylohyoid, geniohyoid, and stylohyoid—also elevate the larynx. On the other hand, muscles like the sternohyoid and omohyoid act to depress (lower) the larynx.
Thus, the actions of extrinsic laryngeal muscles can be grouped into two categories:
Elevators of the Larynx: These muscles raise the larynx
- Thyrohyoid (when hyoid is fixed)
- Stylopharyngeus
- Palatopharyngeus
- Mylohyoid
- Geniohyoid
- Stylohyoid
Depressors of the Larynx: These muscles lower the larynx:
- Sternothyroid
- Sternohyoid
- Omohyoid
Mucous Membranes of the larynx
The mucous membrane of the larynx is continuous with the lining of the pharynx above and the trachea below, forming a smooth passage for air. In certain areas like the posterior surface of the epiglottis, corniculate and cuneiform cartilages, and vocal ligaments, it is firmly attached. In other regions, it is loosely attached, making it prone to swelling.
The laryngeal lining consists of different types of epithelium:
- Squamous epithelium → found on the posterior surface of the epiglottis, upper aryepiglottic folds, posterior commissure, and vocal folds
- Ciliated columnar epithelium → covers most of the remaining laryngeal cavity
- Transitional epithelium → present in some intermediate areas
The vocal folds are covered with squamous epithelium and have a fusiform (spindle-like) shape. Their height decreases towards the front (anterior commissure), contributing to the shape of the subglottic space.
Mucous glands are widely distributed in the larynx, especially on the posterior surface of the epiglottis, aryepiglottic folds, and saccules. These glands produce mucus that helps in lubrication. However, the vocal folds do not contain glands, so they depend on nearby glands for moisture, making them susceptible to dryness (desiccation).
| Laryngeal membranes | Location |
| Mucous membrane (Ciliated Columnar Epithelium) | Present in the entire larynx |
| Cricovocal membrane (ConusElasticus) | Originates from Cricoid cartilage and connects the Cricoid Thyroid and Arytenoid cartilages together. Inserts into the true vocal folds |
| Quadrangular membrane | Connects Epiglottis and Thyroid to the Arytenoid cartilages at the back |
Additionally, a few taste buds are present on the posterior surface of the epiglottis and within the aryepiglottic folds.
Blood supply
The larynx receives blood supply mainly from branches of the superior and inferior thyroid arteries, along with the cricothyroid branch.
The superior thyroid artery arises from the external carotid artery, while the inferior thyroid artery originates from the thyrocervical trunk of the subclavian artery. On the left side, the thoracic duct is closely related to the beginning of the inferior thyroid artery.
The superior laryngeal artery, a branch of the superior thyroid artery, passes deep to the thyrohyoid muscle and enters the larynx by piercing the thyrohyoid membrane along with the internal branch of the superior laryngeal nerve. It supplies the laryngeal muscles and mucous membrane and forms connections (anastomoses) with arteries on the opposite side and with the inferior laryngeal artery.
The inferior laryngeal artery arises from the inferior thyroid artery. It ascends along the trachea with the recurrent laryngeal nerve and enters the larynx below the inferior constrictor muscle, supplying the internal structures.
The cricothyroid artery, another branch of the superior thyroid artery, runs across the cricothyroid ligament and joins with its counterpart from the opposite side.
The venous drainage of the larynx follows the arteries:
- Superior veins drain into the internal jugular vein via the superior thyroid or facial vein
- Inferior veins drain into the brachiocephalic veins through the inferior thyroid vein
- Some blood also drains through the middle thyroid vein into the internal jugular vein
Lymphatic drainage
The larynx has a well-organized lymphatic drainage system. The region above the vocal folds drains through vessels accompanying the superior laryngeal vein, which pass through the thyrohyoid membrane and empty into the upper deep cervical lymph nodes. The region below the vocal folds drains along with the inferior laryngeal vein into the lower deep cervical lymph nodes, often through the prelaryngeal and pretracheal nodes.
The nerve supply of the larynx is provided by the vagus nerve through its two main branches: the superior laryngeal nerve and the recurrent (inferior) laryngeal nerve. The superior laryngeal nerve arises from the vagus and divides into an external branch, which supplies the cricothyroid muscle, and an internal branch, which provides sensory supply to the mucous membrane of the larynx above the vocal folds, including the epiglottis and surrounding areas.
The recurrent laryngeal nerve has a different course on each side of the body. On the right side, it loops around the subclavian artery, while on the left side, it loops around the aortic arch. Both nerves then ascend between the trachea and esophagus to enter the larynx. Inside the larynx, it divides into motor and sensory branches. The motor branch supplies all intrinsic muscles of the larynx except the cricothyroid, while the sensory branch supplies the mucous membrane below the vocal folds. It also gives branches to nearby structures like the heart, trachea, and esophagus.
Voice production
Voice is defined as the modification of the pulmonary (lung) air stream, which means breathing plays a very important role in voice production. During inspiration, the vocal folds remain open, allowing air to enter the lungs. During expiration, especially while speaking, the vocal folds continuously open and close, a process known as vocal fold vibration.
When the vocal folds close, the airflow is momentarily blocked, and when they open, the air is released. This repeated opening and closing converts the continuous airflow into small bursts or puffs of air, which produce sound, known as voice.
Voice has three main parameters:
- Pitch → depends on the number of vocal fold vibrations (frequency)
- Loudness → depends on the force or amount of airflow
- Quality → refers to the pleasantness or characteristics of the voice
Differences between human infant larynx and adult larynx
The larynx and trachea of an infant are much smaller compared to those of an adult. At birth, the infant’s larynx is about one-third the size of an adult larynx. The glottis is narrow, and the vocal cords are short, measuring around 6–8 mm.
In infants, the vocal process of the arytenoid cartilages forms about half the length of the vocal cords, whereas in adults it forms only about one-fourth. The membranous portion of the vocal folds is very small, which is why infants produce a high-pitched, shrill voice.
The laryngeal structures in infants are more flexible and less fibrous, making the airway more prone to narrowing (e.g., due to swelling/edema) and also less easy to feel externally. Additionally, the infant’s larynx is positioned higher in the neck than in adults.
The epiglottis in infants is narrower and often appears tubular or omega (Ω)-shaped, unlike the broader shape seen in adults.
Resonatory system
- Resonators: Pharynx, oral cavity, and nasal cavity
- Together called the vocal tract
- Function:
- Main structure responsible for resonance of speech
- Acts as a filter to modify sound produced by the larynx
- This modification is called the transfer function of the vocal tract
- Components of Resonatory System:
- Pharynx – space above larynx
- Oral cavity – mouth
- Nasal cavity – nose
- Velopharyngeal Port:
- Acts like a door between oral and nasal cavities
- Open → air passes through nose (nasal sounds)
- Closed → air passes through mouth (oral sounds)
- Role: Helps in shaping voice and producing different speech sounds
Articulatory system
- The mouth is an opening through which food and air enter the body. It opens at the lips and leads into the throat.
- There are two cavities in the mouth:
- Buccal cavity
- Oral cavity
- The oral cavity serves as a passage for food and air and contains important structures like teeth, tongue, salivary glands, mucosal glands, hard palate, and soft palate.
- Boundaries of oral cavity:
- Front: Lips
- Sides: Cheeks
- Roof: Hard and soft palate
- Floor: Tongue
- Back: Continues with the pharynx
- The cheeks form the lateral walls, and their inner surface is lined with moist stratified squamous epithelium.
- The oral and buccal cavities are lined with mucous membranes containing small glands (including salivary glands).
- Functions of glands and secretions:
- Keep the mouth moist and clean
- Help in softening food
- Aid in swallowing
- Begin the process of digestion through enzymes
- Overall, the mouth plays an important role in eating, digestion, and speech production.
Tongue
The tongue is a muscular organ present in the mouth. It is the primary organ of taste and plays an important role in chewing, swallowing, and speech production.
Structure: Covered with a mucous membrane. Extends from the hyoid bone (back) to the lips (front). Front upper and lower surfaces are free. Attached to surrounding parts at the sides.
Muscles of tongue: Extrinsic muscles: Attach tongue to external structures → help in movement. Intrinsic muscles: Run in different directions (vertical, transverse, longitudinal) → allow flexibility and precise movements.
Structure features: Upper surface has small projections called papillae → give a rough texture. Contains taste buds, mainly concentrated at the back. Normal color: pinkish-red (changes may indicate health issues).
Functions: Taste: Detects different tastes through taste buds. Chewing: Holds food against teeth. Swallowing: Pushes food into pharynx and then into esophagus. Speech (Articulation): Works with lips, teeth, and palate to produce speech sounds.
| Muscle | Origin | Insertion | Action |
| Extrinsic Muscles |
| Styloglossus | Styloid process | Sides of the tongue | Elevates the tongue |
| Hyoglossus | Hyoid bone | Poster half of tongue | Depresses and elevates the tongue |
| Genioglossus | Genial tubercle of Mandible | Tip-base of tongue, Hyoid | Protrudes tongue, raises Hyoid |
| Palatoglossus | Soft palate | Poster and lateral aspects of tongue | Elevates the tongue |
| Intrinsic muscles |
| Superior Longitudinal | Root of the tongue | Tip of tongue | Shortens and curles tongue |
| Inferior Longitudinal | Root of the tongue | Tip of tongue | Shortens and curls tongue downwards |
| Transverse | Lingual septum | Dorsum, lateral margins of tongue | Elongates; raises and narrows sides of tongue |
| Vertical | Dorsum of tongue | Lower surface of tongue | Flattens and broadens tongue |
The oral tract can be imagined as a box, where the tongue forms the base, the palate forms the roof, and the teeth and lips form the front. Among these, the tongue and lips are movable, allowing changes in shape. Although these organs are mainly used for chewing, they play a crucial role in speech production.
The oral tract is about 17 cm long and acts like a filter for sound. When voice (produced by vocal folds) enters the oral tract, it contains energy at different frequencies. The oral tract modifies this sound by allowing some frequencies to pass and absorbing others, similar to a sieve.
Different speech sounds are produced by changing the position of the tongue. For example, while producing /g/, the back of the tongue touches the palate, dividing the oral tract into two parts. When producing /d/, the tongue position changes, creating a different shape of the oral cavity (filter).
Thus, speech = voice + filter (oral tract function). Different tongue positions create different filters, which result in different speech sounds. Without the oral tract, it would not be possible to produce a variety of speech sounds.
Lips
The lips are one of the most visible and expressive organs of the human body. They are made up of skin, muscles, and mucosa. The upper lip (labium superioris) is usually smaller than the lower lip (labium inferioris). The vermilion border is the colored area that separates the lips from the surrounding skin, and the philtrum is the vertical groove above the upper lip. The reddish color of the lips is due to underlying blood vessels.
Lips are delicate structures because they do not have hair, sweat glands, or oil (sebaceous) glands for protection. They are controlled by facial muscles, mainly the orbicularis oris, which helps in lip movement.
The main functions of lips include taste (gustatory function), closing the mouth tightly, protecting from unwanted objects, and importantly, helping in speech production by forming different sounds.
Teeth
The teeth play an important role in chewing (mastication) by tearing and grinding food into smaller pieces for digestion. An adult has 32 teeth (16 in the upper jaw and 16 in the lower jaw). Each tooth has two main parts: the crown (visible part) and the root (embedded in the jaw), which meet at the neck near the gum line.
The crown consists of three layers: enamel (outer protective layer), dentin (main body of the tooth), and pulp (inner part containing nerves). The root helps to anchor the tooth firmly in the jaw.
Although the primary function of the teeth and related systems is chewing, breathing, and protection, they also assist in speech production. For example, teeth help in producing certain speech sounds clearly. Since these organs are not originally meant for speech but support it, speech is called an “overlaid function.”
Palate
The palate forms the roof of the mouth and separates the oral cavity from the nasal cavity, allowing separate pathways for air and food. It has two parts: the hard palate (anterior, bony) and the soft palate (posterior, muscular).
During speech production, different parts of the oral cavity have specific roles. The hard palate, alveolar ridge, and teeth act as sound reflectors, while the soft palate (velum), cheeks, lips, and tongue act as sound absorbers.
Because of this combination of sound reflection and absorption, along with the ability to change shape and size, the oral cavity becomes a highly versatile resonator, helping to produce a wide variety of speech sounds.
Hard palate
The hard palate is the bony front part of the roof of the mouth, usually pale pink or whitish in color. It is formed by four bones: the palatine processes of the maxilla (anteriorly) and the horizontal plates of the palatine bones (posteriorly). These bones join together during development at the midline called the palatine raphe. The hard palate is covered by a mucous membrane.
It plays an important role in swallowing, and is crucial for speech production, especially for resonance and articulation of certain sounds (like palatal and retroflex sounds).
If the palatal bones fail to fuse properly during development, it leads to a cleft palate, which can cause problems in speech and resonance. Some children may have a high-arched palate, which can also lead to articulation errors.
A bluish tint at the midline may indicate a submucous cleft, which affects normal speech production. Thus, the hard palate is essential for both normal speech and feeding functions.
Soft palate
The soft palate (velum) is a muscular extension of the hard palate, covered by mucous membrane and rich in blood supply, giving it a reddish color. At its posterior end is a small conical projection called the uvula.
The palatine aponeurosis within the velum helps in velopharyngeal (VP) closure, which is important during swallowing and speech. During swallowing, the soft palate and uvula move upward, closing the passage between the nasopharynx and oropharynx, thus preventing food or liquid from entering the nose.
On either side of the uvula are two folds: the glossopalatine arch (anterior) and the pharyngopalatine arch (posterior). The palatine tonsils, located between these folds, help in defending the body against infections.
In speech production, the velum plays a key role in resonance. It is raised (VP port closed) during oral sounds to prevent air from escaping through the nose, and lowered (VP port open) during nasal sounds to allow airflow through the nasal cavity.
If the soft palate muscles are weak or paralyzed, it may lead to hypernasality, where excessive air passes through the nose during speech.
| Muscle | Origin | Insertion | Action |
| Tensor Veli Palatini | Scaphoid fossa, Eustachian tube | Palatine aponeurosis | Tenses soft palate |
| Levator Veli Palatini | Petrous portion of Temporal bone | Palatine aponeurosis | Raises soft palate |
| Uvulus | Postr nasal spine, Palatine aponeurosis | Mucosa of Uvula | Shortens Uvula |
| Palato-glossus | Under surface of soft palate, Palatine aponeurosis | Dorsum and sides of tongue | Elevates tongue and narrows palatine arches |
| Palato-pharyngeus | Palatine aponeurosis | Pharyngeal walls; Thyroid cartilage | Consticts palate-pharyngeal folds |
Nasal cavity and Nose
The nasal cavity plays an important role in filtering and cleaning the air before it reaches the lungs. It is lined with respiratory mucosa, which contains tiny hair-like structures called cilia. These cilia move in a wave-like motion to push mucus (containing dust, bacteria, and harmful particles) towards the throat for removal.
The floor of the nasal cavity (which is also the roof of the mouth) is formed by the hard palate, consisting of the palatine bone and maxilla. The olfactory membrane, located on the roof, contains receptors for the sense of smell, connected to the olfactory nerve and bulb.
The nasal cavity is divided into two parts by a vertical structure called the nasal septum. The nose is made up of bones and cartilage, with the bridge formed by nasal bones and maxilla. Air enters through the nostrils (external nares) and passes through the nasal cavity to the nasopharynx via internal nares.
Thus, the nasal cavity is essential for breathing, filtering air, and smelling.